Page contents
The information here will help you understand your wrist injury, guide you through your rehabilitation and explain what you can do to maximise your recovery.
Advice for a recent wrist injury
In the first 72 hours, it’s important to:
- rest your wrist
- elevate your wrist using a pillow, cushion or sling
- apply a cold pack regularly
- protect your limb by wearing your sling and/or plaster cast
It’s helpful to remember PRICER:
- Protect
- Rest
- Ice
- Compression
- Elevate
- Rehabilitation
Medication
The Emergency Department (ED) or a Minor Injuries Unit (MIU) may have prescribed you with some pain relief. Take these as instructed to help manage the pain.
If you do not feel that this medication is helping, talk to us during your appointment in Fracture Clinic, or your GP, about an alternative option.
Cold packs
Ice is a great natural anaesthetic that helps relieve pain and controls swelling. Apply ice packs or a bag of frozen peas wrapped in a wet thin towel to your injured area for up to 15 minutes every few hours.
- Do not place ice in direct contact with the skin.
- Do not leave the ice pack on for more than 20 minutes at a time in one hour.
Rest and elevation
It’s important to rest your injured area as much as possible in the first 24 to 72 hours.
It’s normal to experience swelling after your injury which is often worse at the end of the day.
Elevation reduces swelling, which in turn relieves pain and speeds up your healing. Keep your injured area elevated as much as possible during the first 24 to 72 hours.
If you have been given a sling, use it to keep your injured area elevated. You may find it more comfortable to use pillows to elevate it during the evening and at night.
If you have a lower limb injury, try to keep your feet elevated above the level of your hip.
Smoking
Medical evidence suggests that smoking prolongs fracture healing time. In extreme cases it can stop healing altogether. Stopping smoking during the healing phase of a fracture will help ensure optimal recovery from this injury.
For advice on stopping smoking and local support available, please discuss this with your GP or go to the NHS Smoke Free website.
Helping your recovery
Being healthy can help you recover from your injury faster. Eating well, staying hydrated and keeping as active as possible will all help. We’ve put together a set of videos on all the things you can do to help you recover as quickly as possible.
If you need an operation
In some cases you may need an operation to realign your bones. This may involve putting wires, plates, screws or rods inside your arm. Sometimes we may need to use a temporary external frame.
What are the risks with surgery?
If you’re overweight, smoke or not active, you’re at greater risk of developing complications after surgery. It may take longer to recover.
Possible complications that you should be aware of include:
- scarring on the wrist
- tendon, nerve or vessel damage around the wrist joint
- infections, which we can treat with antibiotics
- further surgery if wounds become more deeply infected
- nerve pain (in rare cases) which may need further treatment
- further surgery if the fracture is not stable or does not heal properly.
Most complications are minor and can be treated easily and successfully.
How long will I spend in hospital?
Wrist surgery patients generally go home the same day. You may need to spend one night in hospital.
After surgery you’ll need to strictly rest and elevate your arm. You can expect to be up and active within 48 hours. Your surgeon will tell you more about this.
Managing your injury after surgery
You may need a sling to protect your wrist and manage swelling. Use it for 1 to 2 weeks, but no longer as it’s important that your elbow doesn’t get stiff.
More information about having an operation
You can find out more about having an operation on our surgery for fractures and soft tissue injuries page.
Care plan
The information below will help you understand your injury, guide you through your rehabilitation and explain what you can do to maximise your recovery.
Your diagnosis should have been made by an orthopaedic consultant or one of the team working under the supervision of the consultant team. The information in these care plans is to help you understand your diagnosis and is not exhaustive.
Non-urgent advice: Please note:
Your consultant may give you a different, personalised care plan based on your injury and whether you need imaging (x-ray, CT scan, MRI, or an ultrasound) or an operation.
Wrist fracture
What is your injury?
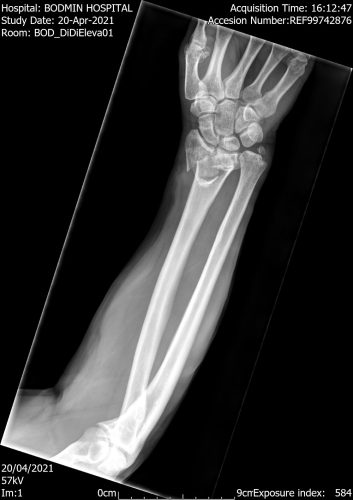
You have broken one or two bones in your wrist:
- The radius, which is on the side of your thumb,
- the ulna, which is on the side of your little finger,
- or both.
These are among the most common injuries we treat in fracture clinic.
They’re usually caused by a fall on an outstretched hand that forces the wrist backwards. They’re common in young children and older people.
Healing
It normally takes up to 12 weeks to heal, and longer to regain full strength and movement, but this may differ depending on your individual circumstances. For example, children heal quicker than adults. We’ll discuss how long we expect your injury to take to heal with you, and whether you’re likely to need an operation.
If you don’t need, or choose not to have an operation, you’ll be in a plaster cast for 4 to 6 weeks (children will need a cast for less time as they heal quicker, usually less than five weeks).
It is important not to put any weight through your wrist for 6 weeks after your injury. You can put weight through your elbow.
Follow up
If we need to follow up with you, either on the phone or face to face, we’ll contact you by phone to arrange. If you need an operation, we’ll discuss this with you and help you make an informed decision
You can also book an open appointment to see someone about your wrist at any time in the 6 months after your injury. Please call 01736 758892 to make an appointment.
Please call the Fracture Clinic on 01872 253091 if:
- you’re unable to follow this rehabilitation plan
- you have any questions
- you’re struggling with your sling
- you notice pain in an area other than your wrist.
Early movement and exercises
Wrists get stiff very quickly. Keep your fingers, elbow and shoulders moving as normal while you are wearing your cast.
The exercises here will help you regain range of movement in your wrist, hand and elbow.
Exercises to do whilst in your plaster cast
Exercise 1
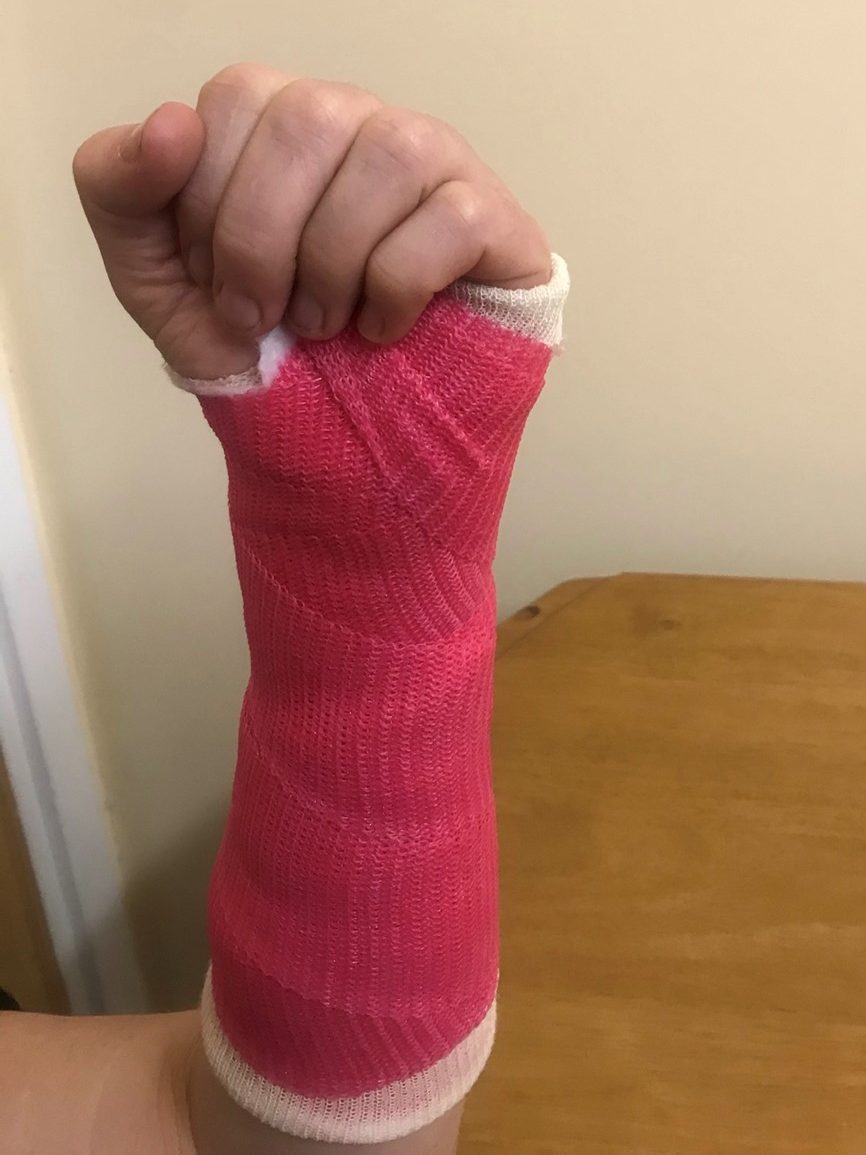
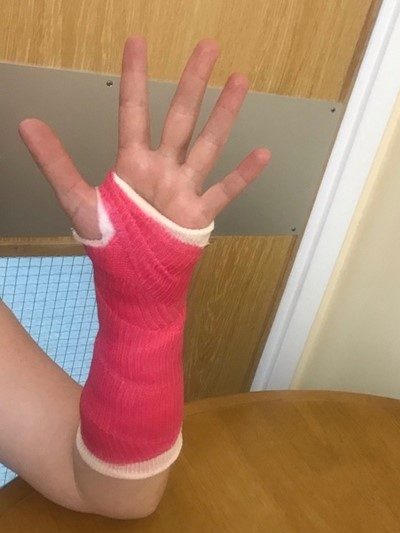
Support your elbow on a table with your wrist straight and your fingers pointing towards the ceiling.
Make a fist with your thumb over your fingers.
Straighten your fingers and bring them apart. Repeat 10 times.
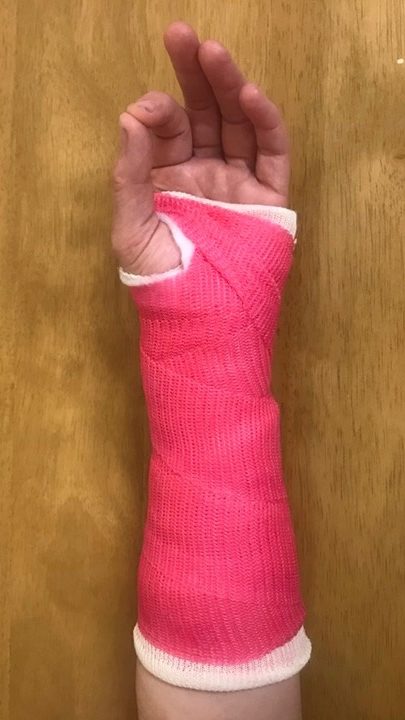
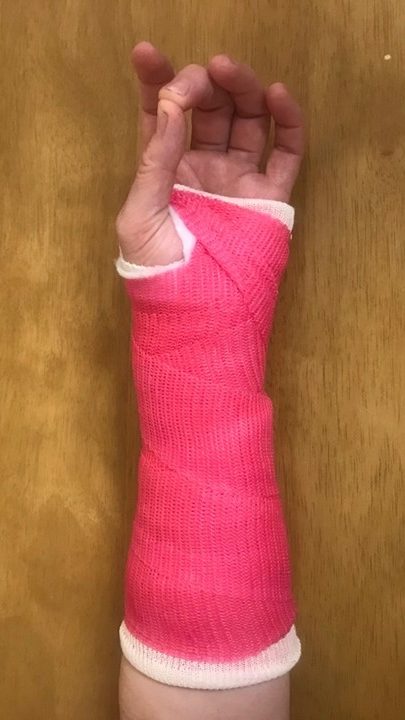
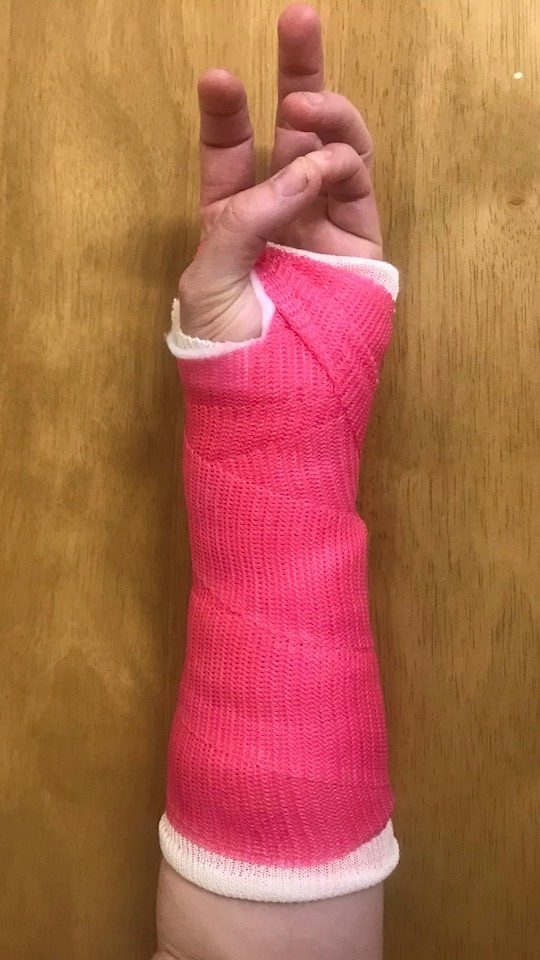
Exercise 2
Put the back of your hand on a table.
Bring your thumb to the base of your little finger. Continue to bring your thumb to touch the base of each finger. Repeat 10 times.

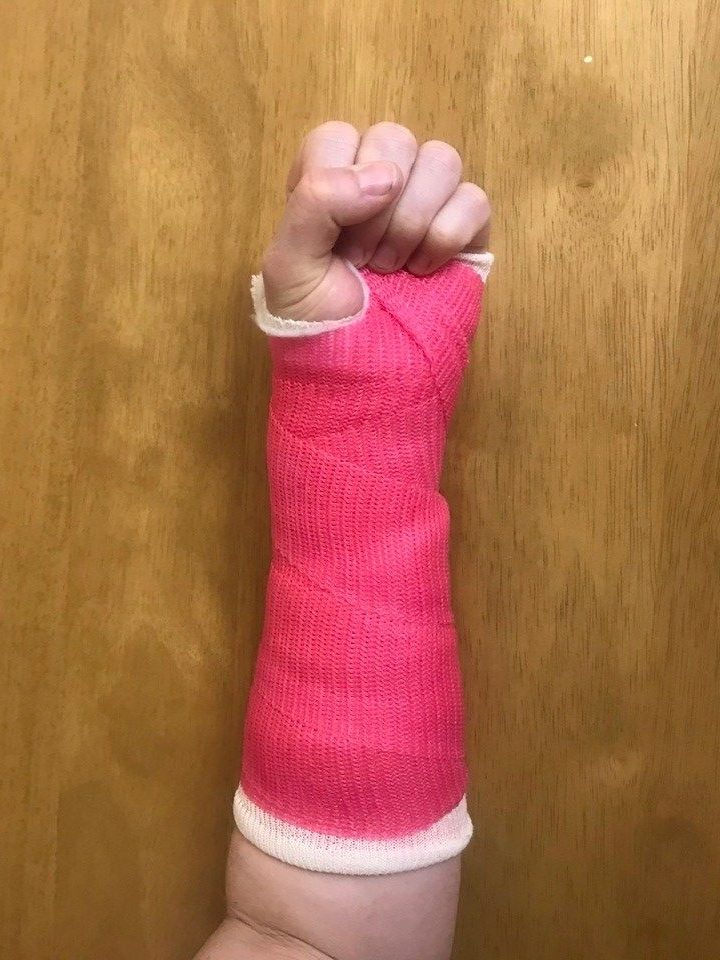
Exercise 3
Make a fist.
Extend your thumb away from your fingers and then draw it close over the top of closed fingers. Repeat 10 times.
You may not be able to do all of these, depending on your particular cast.

Wrist and hand exercises for after your cast or splint has been removed
Do these exercises every day for 6 weeks once your cast or splint has been removed. These exercises increase in intensity, so work through at your own tolerance.
Try to complete all exercises.
You should:
- take painkillers 20 to 30 minutes before starting your exercises
- complete the exercises on both wrists
- do the exercises little and often
- start with your forearm resting on a table to make it easier
- expect some discomfort (but sharp pain and increased swelling indicates you’re overdoing it).
Exercise 4
Place the palm of your hand on a table.
Bring your thumb away from the index finger and then back again.
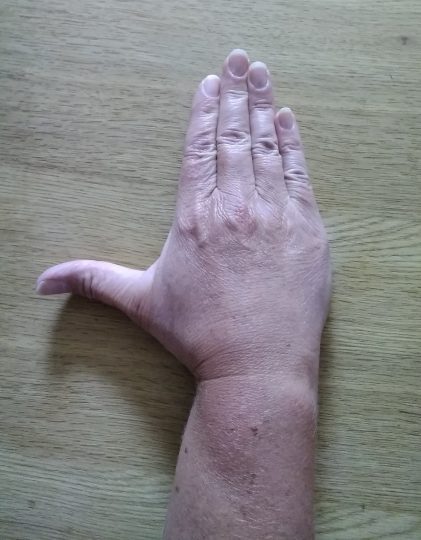
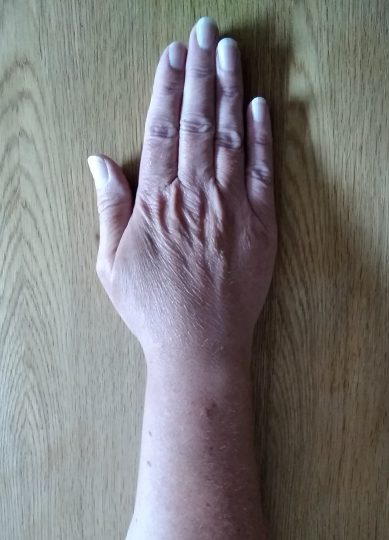
Exercise 5
Fully bend your wrist forward 10 times. Try to bend your wrist a little more. Hold for 30 seconds.
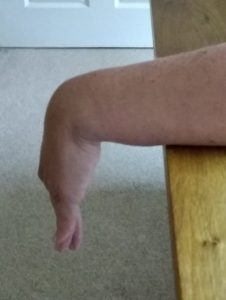
Exercise 6
Fully straighten your wrist upwards 10 times. Try to straighten your wrist a little more. Hold for 30 seconds.
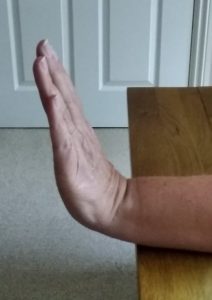
Exercise 7
Rest your forearms on a table, palm turned down. Alternate turning the palm up and down. Repeat 10 times.

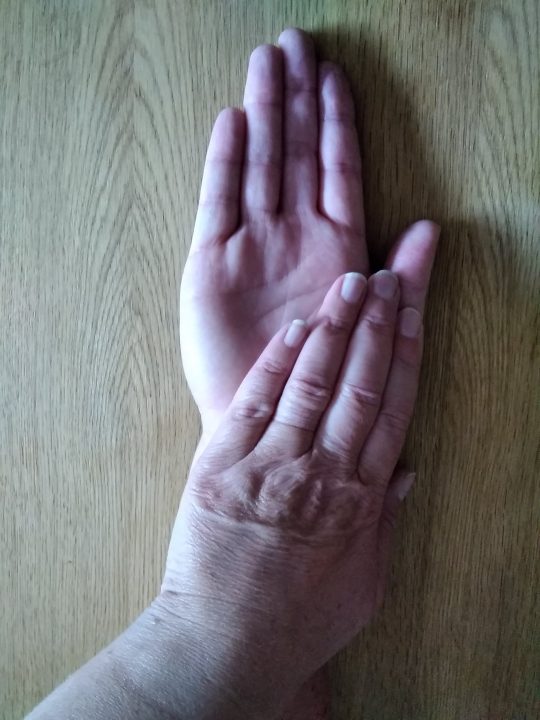
Tip: For exercises 5, 6, and 7, you can use your other hand to gently assist your injured wrist.
Exercise 8
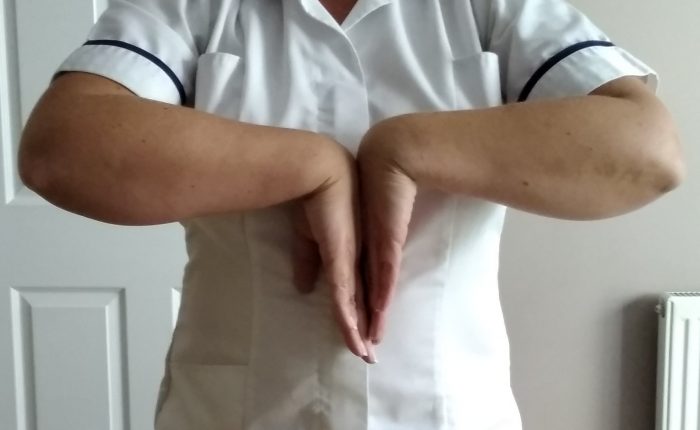
Bring your hands into prayer position with your fingertips pointing towards the ceiling. This may be difficult at first but with practice it should become easier.
Try to keep your hands in prayer position but reverse it with your fingertips pointing towards the ground. Repeat 10 times.

From 12 weeks after your injury
Do these when you have regained maximum range of motion, you’re pain free, and 12 weeks have passed since your injury.
Grip strength
Squeeze a soft ball in your hand. Hold for up to 30 seconds. Repeat 5 times.
Using a small weight
Practice exercises 5, 6, and 7 using a small weight (such as a can of baked beans or something less than 0.5 kg) or a pair of tights tied to something for a little resistance.
Preventing complications
Caring for your wound and stitches
If you’ve had an operation, you’ll need to keep your stitches dry and clean. You should also look out for any redness or signs of swelling, bleeding or pus as these can be signs of an infection.
You can find information about how to care for your stitches, if/when they need to be removed and signs of an infection on our surgery for fractures and soft tissue injuries page.
Blood clots and Deep Vein Thrombosis (DVT)
Because your limb is immobilised and you’ll be moving less than normal, you’re at higher risk of developing a blood clot or Deep Vein Thrombosis (DVT). This can be life threatening if left untreated.
Symptoms of DVT in the leg are:
- throbbing or cramping pain in 1 leg (rarely both legs), usually in the calf or thigh
- swelling in 1 leg (rarely both legs)
- warm skin around the painful area
- red or darkened skin around the painful area
- swollen veins that are hard or sore when you touch them.
These symptoms can also happen in your arm or tummy if that’s where the blood clot is.
More information about DVT
- Watch this video about how to prevent DVT.
- Learn more about DVT including symptoms, who is at risk and how to treat it.
- Find out how to reduce the risk of blood clots when you have an immobilised lower limb (PDF, 108 KB).
Preventative medication for DVT
If you have been told not to put any weight through your leg or to partially weight bear (50%), you should have been assessed in ED or MIU and told if you need to take preventative medication.
If you have not had this conversation please call your GP for an urgent appointment.
Depending on your injury, you may have been prescribed a course of a blood thinner. There are a few different types of medication and they often need injecting into your tummy. You can discuss an alternative with a doctor. Please see the relevant care plan for your injury.
Pressure sores and ulcers
Wearing a boot or plaster cast combined with not moving your limb can lead to pressure sores or ulcers. These are injuries to the skin and underlying tissue caused by prolonged pressure, rubbing or tension.
They often develop gradually, but can sometimes form in a few hours.
Signs and symptoms of pressure sores
These include:
- skin discolouration – red patches for people with pale skin, purple or blue patches for people with dark skin
- discoloured patches that do not turn white when pressed
- a patch of skin that feels warm, spongy or hard
- pain or itchiness in the affected area.
If you have a boot, take it off every day to check your skin and make sure it’s not rubbing.
If you have a plaster cast, look out for a change in colour (red or white) of your skin above or below the plaster, an increase in pain inside the plaster or pins and needles.
- Watch this video to learn how to prevent pressure sores.
- Read more about pressure sores on the NHS website.
If you think you have a pressure sore or ulcer call the Fracture Clinic straight away on 01872 253091.
For out of hours advice please call 01736 758909.
Sepsis
Sepsis (also known as blood poisoning) is a serious infection that can be life threatening. There is no one sign for sepsis so it can be hard to spot.
Call 111 immediately if you develop any of the following:
- Slurred speech or confusion
- Extreme shivering or muscle pain
- Passing no urine in a day
- Severe breathlessness
- It feels like you’re going to die
- Skin is mottled or discoloured.
Find out more about the symptoms of sepsis on the NHS website.
These videos also explain what sepsis is and how to spot the early signs.
Living with your injury
Driving
Wait at least two weeks after your injury or surgery. After that, you can return to driving when:
- you have been told you no longer need your sling
- we’ve removed your cast (if you had one)
- you’re able to turn the steering wheel comfortably and without any pain
- you can control the vehicle safely
- you’ve checked it’s okay to drive with your insurance company.
Always test your ability to drive with the ignition off and in a safe environment.
If you have a follow-up appointment with us, please wait until your consultant or physiotherapist has given you clearance to drive. If you are in any doubt, do not drive until you have spoken to our team.
Work
Decisions to return to work are made on a unique basis and should be discussed with the Fracture Clinic, your GP and your employer.
You may need time off work and when you return, you may need light or amended duties. When you should return to work will depend on your profession and your injury.
You can get a fitness to work statement or a sick note when you come into the Fracture Clinic. If you don’t need to come and see us, you can get one from your GP.
Sport
You should not do any sports or heavy lifting for at least 12 weeks, but possibly longer, depending on your injury.
Thank you to Brighton and Sussex University Hospitals for kindly letting us use information from their care plans to create this site.
Page last reviewed: 30 January 2024